Approximately 12,000 new cases of cervical cancer occur each year in the United States, and about 1/3 of these people will die from it. This deadly cancer, that tends to strike young women, is usually preventable by having regular Pap tests. This cancer is thought to be due to human papillomavirus, a common virus that can cause warts and also abnormal cells that progress toward cancer.
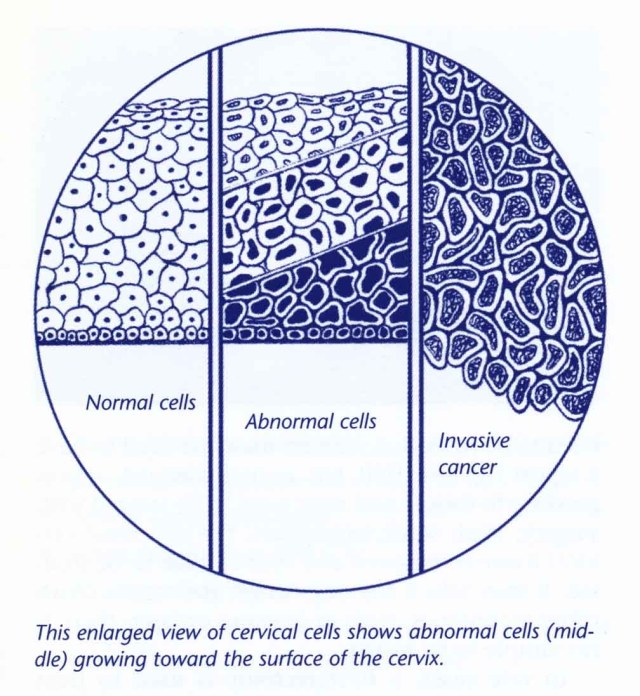 The cervix (the part of the uterus that is located at the top of the vagina) is covered by many thin layers of cells. These healthy cells normally slowly grow and are replaced over time. Cancer occurs when the rate of growth of these cells changes and becomes unregulated. The abnormal cells tend to arise from a vulnerable part of the cervix where the cells on the inside of the cervix (called columnar) meet the outside cells (called squamous). The “squamo-columnar junction” is a site where slowly, over years, cells can go through different stages of abnormality, culminating in the formation of cancer cells that make up a tumor which can spread to other organs in a harmful way. Fortunately, it takes years for the cancer cells to develop, and we have many opportunities along the way to detect them by simple pap smears and other more advanced testing.
The cervix (the part of the uterus that is located at the top of the vagina) is covered by many thin layers of cells. These healthy cells normally slowly grow and are replaced over time. Cancer occurs when the rate of growth of these cells changes and becomes unregulated. The abnormal cells tend to arise from a vulnerable part of the cervix where the cells on the inside of the cervix (called columnar) meet the outside cells (called squamous). The “squamo-columnar junction” is a site where slowly, over years, cells can go through different stages of abnormality, culminating in the formation of cancer cells that make up a tumor which can spread to other organs in a harmful way. Fortunately, it takes years for the cancer cells to develop, and we have many opportunities along the way to detect them by simple pap smears and other more advanced testing.
Human papilloma virus (HPV) is now thought to be a major cause of many types of cancer, including the cervix, anus, vulva, vagina, head, neck and throat. There are many different subtypes of HPV; about a hundred have been identified. These have been separated into different groups according to risk. HPV infection is very common. It is usually passed from person to person by sexual contact, both genital and oral. Recently a study of 5600 men and women ages 14 to 69 showed a large prevalence of oral HPV infections, particularly in sexually active men. Oral HPV infections were three times more common in men (10.1%) than in women (3.6%), and were highest among those who smoke at least 1 pack a day and had more than 20 lifetime sexual partners.
Even though HPV infection is very common, being infected with HPV does not necessarily mean that a person will get genital warts or develop cancer. Usually a woman’s immune system will attack the HPV virus quickly, and clear it from her body. In a small number of women the HPV does not go away and it becomes a persistent infection. This can occur if the person’s immune system is not as strong, such as one that is weakened by smoking, or if the virus is particularly virulent. The longer the virus is present, the more it can harm the cells of the cervix.
Currently we have vaccines available to protect against some types of HPV, particularly the 2 that most often cause cancer. The vaccines strengthen the person’s immune system to fight the virus. The vaccines require 3 injections that are given over six months. They are approved by the FDA for use in females and males from 9 to 26, but can be given to men and women of all ages.
There are risk factors for cancer of the cervix, depending on your sexual history, your health and your lifestyle. The more important risks are having multiple sexual partners, having a male partner who has had multiple sexual partners, having sex at an early age (less than 18), smoking, and a family history for cancer.
Symptoms of cervical cancer do not occur early when the disease is in the pre-cancer state, known as dysplasia. In early stages there are no symptoms. Dysplasia of the cervix is detected by pap smears, confirmed by biopsy, and treated very successfully by simple procedures. The biopsy that is performed in the case of an abnormal pap test is called a colposcopy. This is an examination of the cervix with magnification that we perform in our office, analogous to looking at the cervix with a magnifying glass. The most abnormal area is selected and a biopsy is taken. The results may be normal, or they may confirm that pre-cancer (dysplasia) of the cervix is present. If pre-cancer of the cervix is confirmed, it may be present in mild, moderate, or severe forms. These pre-cancerous conditions are treated by the LEEP procedure. The LEEP is performed as an out-patient procedure and requires anesthesia. It involves removing a very small portion of the tip of the cervix, about the size of a nickel, and the tissue specimen is sent out for analysis by a pathologist. The study of the tissue will reveal if the pre-cancer was removed entirely and if the final report is the same as the biopsy, better, or worse.
Unfortunately, in some cases cervical cancer may be diagnosed. Because it can spread to other areas of the body, extensive testing is usually performed before the correct treatment is chosen. These tests can include ultrasound, computerized tomography (CT scan), magnetic resonance imaging (MRI) or positron emission tomography (PET scan).
Staging is the process of finding out how much the cancer has spread. The staging is from 0 to 4, with the higher numbers indicating more spread of the tumor, and more need for treatment. Treatment works best in the early stages of the disease. The 5 year survival rate for Stage 1 is 91%, compared with 17% for Stage 4.
There are many treatments for cervical cancer, and the success of these treatments is improving all the time. It is best, however, to avoid cancer rather than be treated for it. There are many ways you can decrease your chance of developing cancer: not smoking, getting the vaccine against HPV, having a smaller number of sexual partners, using condoms when you are single, and having routine pap tests. If you have questions about cervical cancer, pre-cancer, or warts, ask us (or your doctor) when you come in for your next office visit.
Reference: The American Congress of Obstetricians and Gynecologists


Pingback: Sex Statistics.Live Science. « Ramani's blog
Pingback: Cervical Cancer Is Preventable | WWW.SHOAIBGARANA.COM
Pingback: Carcinoma Cervix « MD/MS/DNB
Pingback: AIDS | WEBSITEPOINT.NET