 I’m going to start a series of articles about cancer. This subject is scary to everyone, but the more you know about it, the safer you are. Almost every week I see someone who had cancer or pre-cancer previously, and now is all better and back to normal. There has been tremendous progress in the detection of many types of cancer, and the treatment of them is much improved over what it used to be. Someone once told me the job of an ObGyn is to check every patient for cancer. When I see patients I always think of that. I’m going to write about it so the knowledge can make you safer. I have to say, though, that this blog is not intended as specific medical advice for your particular condition. If you think you have a breast lump or problem or concerns about cancer, you should see someone about it.
I’m going to start a series of articles about cancer. This subject is scary to everyone, but the more you know about it, the safer you are. Almost every week I see someone who had cancer or pre-cancer previously, and now is all better and back to normal. There has been tremendous progress in the detection of many types of cancer, and the treatment of them is much improved over what it used to be. Someone once told me the job of an ObGyn is to check every patient for cancer. When I see patients I always think of that. I’m going to write about it so the knowledge can make you safer. I have to say, though, that this blog is not intended as specific medical advice for your particular condition. If you think you have a breast lump or problem or concerns about cancer, you should see someone about it.
Today’s topic is Detecting and Treating Breast Problems.
Your breasts are made up of glands, fat and fibrous tissue. They respond to changes in hormones estrogen and progesterone during your menstrual cycle. This can result in a change in the amount of fluid in the breast that can make the fibrous areas more painful. Breasts also change during pregnancy, breastfeeding and menopause. You may notice changes in your breasts due to hormonal birth control, such as the pill or the ring, during hormone therapy, or if you have breast implants.
Most breast problems, especially in younger women, are benign. Common symptoms include lumps, discharge from the nipple, or pain. Common breast problems include fibrocystic changes, cysts and fibroadenomas. Fibrocystic changes are changes that cause a woman’s breast to feel lumpy and tender. This can cause pain, itching and swelling, and usually occurs in both breasts. It frequently will become worse before a menstrual period and better after it is over. Cysts are small sacs filled with fluid. They can change with the menstrual cycle and are most often found in women between 25 and 50 years of age. Fibroadenomas are solid, benign lumps often found in young women. On physical exam they have a “slippery” feeling. Most women who have any of these problems do not have cancer, but you should let us know if you find something suspicious in your breasts. A physical exam and tests can help us find out what is there and what needs to be done about it.
Breast self-exam is something you can do to help find a lump or a change in your breasts.

A series of six illustrations showing how to do breast self examination (BSE) (Photo credit: Wikipedia)
We usually recommend doing it after each period, or once a month if you are beyond the menopause. First you look at yourself in good light in front of a mirror. Look for dimpling, puckering, or redness of the breast. Then lie flat on your back and using your sensitive fingertips search one breast and then the other. If you think you have found a lump, you compare it with the same area on the opposite side, the “mirror-image” of it. If you can find something there that is similar, it may turn out to be normal tissue. You also look for a “dominant lump,” or one that is larger than the other normal-sized lumps, and you look for a lack of symmetry from side to side.
Breast problems are evaluated by physical exam, and by testing that includes breast ultrasound, mammography and MRI. We perform a clinical breast exam in our office at least once a year. We check for changes in size or shape, we look for dimples or redness of the skin. We feel for lumps that are larger than they should be, and we compare one breast with the other looking for a lack of symmetry. We check for enlarged lymph nodes. We look for a bloody nipple discharge. We look for areas of tenderness. In most cases an exam will be normal and no further testing is needed. In some cases, however, we send the patient to have more evaluation by breast ultrasound, x-ray or magnetic resonance imaging (MRI).
Breast ultrasound is a test using sound waves at a high frequency that create a picture of the inside of your breast. It is especially useful for determining if the interior of a lump is cystic or solid. Sometimes cysts are found, and the fluid within them can be aspirated out with the result that the cyst goes away. The fluid can be sent for analysis if there is a question about it. Often cysts will come and go with the menstrual cycle, and they do not have to be removed.
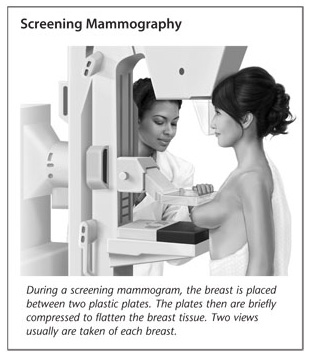
Mammography is used to examine breast tissue by x-ray. It should be done yearly starting at age 40, or sooner if you have factors that increase the risk of breast cancer such as genetic predisposition, or previous abnormal biopsy results. Mammography can find tiny lumps before they can be felt. We had a patient who had cancer detected by it and the size of the cancer turned out to be just 3 mm in size, about as large as a grain of rice. Cancers detected so early frequently can be cured by relatively simple and quick treatment. Mammography will also be used over time. The films from your first study are saved and are compared with later ones to more accurately detect changes. The test can sometimes be uncomfortable for you. It is less painful to have the test done after a period rather than before or during one.
There are two types of mammography, the routine screening test, or the diagnostic one. If you are going for a routine yearly mammogram you have the screening type, which uses fewer images. If you are having it done to answer a question about a symptom or lump, then the diagnostic one is more thorough and will give a specific answer in a detailed report. Another type of mammography you may hear about is digital mammography. This differs from standard mammography in the way the image is stored. Instead of x-ray film, the image is converted into a digital file and is stored on a computer. It may be enlarged or enhanced by a computer program. Digital mammography may be better at detecting cancer in some groups of women, such as those with more dense breast tissue.
The main downside to mammography is that it is not always accurate. It’s estimated that about 10% of cancers cannot be detected by mammography. So if you have a lump, and even though the mammography came back “normal,” you should call us about it if you believe it is becoming larger. Breast lumps that are becoming larger can be cancer, whether the lump hurts you or not.
A new test to evaluate the breast is MRI. Magnetic resonance imaging uses a strong magnetic field to create a detailed image of the inside of the breast. Women who have a high risk of breast cancer may have MRI in addition to mammography for breast cancer screening. This high risk refers to someone with a mutated BRCA gene as detected in a genetic test for breast cancer. MRI is not recommended for screening to detect breast cancer in all women because it is not as good as a mammogram for certain breast conditions, such as ductal carcinoma in situ (a type of early breast cancer).
If a lump or other problem is detected a fine-needle biopsy or surgical biopsy may be the next step. In that case the biopsy will obtain a small piece of tissue that will yield a definite result as to what the tissue represents. The results are reliable and will usually determine if the tissue is benign (not cancer) or if cancer is present and treatment is needed.
I hope this information has been helpful to you in getting a better understanding of the types of common breast problems that can occur, and how we evaluate them to detect those that are benign or malignant. In most cases the results are good and we can give reassurance that the problem is not a serious one. In some cases the results show cancer, but the treatment is available and very effective.
Breast cancer is a scary subject for all of us. We have many patients who have had breast cancer that was successfully treated. I see them year after year and they continue to be in good health, even 20 or 30 years later. Sooner or later you will hear of a close friend or co-worker who just found out that they have breast cancer. 10% of the female population will eventually get it. If you check yourself monthly, and have regular exams and screening tests you will be likely to have early detection and early cure, should it ever be discovered in your breast.
Reference: American Congress of Obstetricians and Gynecologists at http://acog.org